Karin Transplant Journey, Part 2: The Dialysis Cleanse

Since studying diabetes in medical school, I have been awfully afraid of kidney disease. The complications of diabetes both scare and fascinate me – so much that I went on and did a PhD in diabetic complications followed by a post doc at Harvard studying the same. I had an almost obsessive fascination with the issues I might face in the future, if I were unlucky.
25 years later I am on dialysis – the ultimate, final step in kidney failure treatment. Dialysis implies the kidneys are no longer working, even minimally, and a machine needs to take over the very important functions normally executed by those bean (or as my daughter has come to name them “croissant”) – shaped organs.
The kidneys do more than excrete urine. In fact, many of the functions are not well known to most, including their importance in blood pressure regulation, hemoglobin production (which carries oxygen to all tissues), calcium and phosphate metabolism and electrolyte regulation. However, what most of us know is that kidneys filter out toxins and break down certain drugs and compounds. That means that if the kidneys don’t work well, you literally become toxic (uremic) and those compounds that are meant to be broken down in the kidneys remain at very high levels in the blood.
I was facing dialysis in April of 2023, due to a few unfortunate events that can be seen as cautionary (and, by me, as detrimental). I had been planning my second kidney transplant for a while. I had lots of time to speak to my donor (my sister), get used to the idea of going through surgery again and plan for the recovery carefully. However, during my cardiac evaluation, an errant stress test triggered a confirmatory angiogram, which luckily was negative for blockage. But this test (angiogram) used a contrast agent which led to my kidney failing rapidly and acutely.
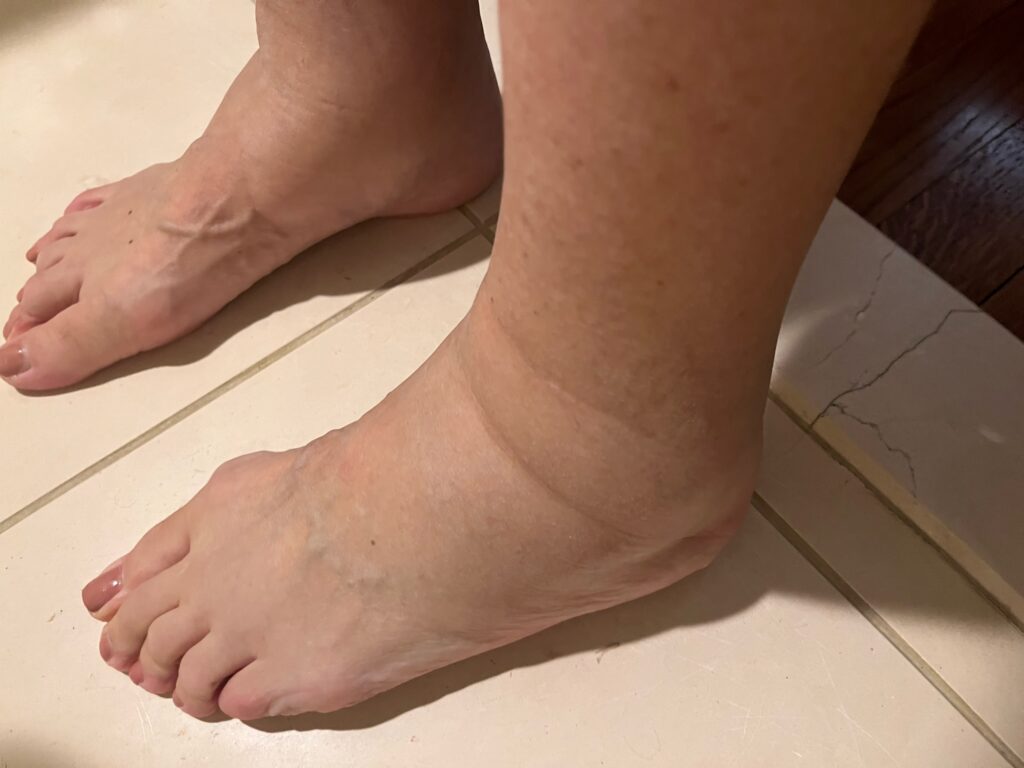
I started feeling very differently than before. My chronic fatigue that I was getting used to was worse. My sensitivity to cold was complemented by nausea, itching, persistent high blood pressure (sky-high levels), followed by headache and blurred vision. I was uremic and so swollen that my clothes did not fit, and I was very uncomfortable.
I had to be emergency-hospitalized, and right before my first dialysis session, I was more scared than I have been of anything in my life.
I had pictured the scenario many times, a machine taking over from my kidneys, vacuuming my blood out, filtering and cleaning it, then pushing it back into my vessels. I envisioned myself hooked to a machine, without which I would slowly die of internal poisoning.
The reality was that my first session was in a low-lit room at Columbia Presbyterian hospital, in a comfortable bed, with a Samsung screen in front of me, and a gentle nurse who took me through the process. Three hours later, I was rolled back to my room. It was not that bad!
I went through another two sessions in the hospital, one a day, which is very aggressive, but my toxicity levels were bad and I needed detoxification desperately to get ready for my transplant.
When I was released, I had to go to dialysis in an out-patient setting, and the scenario was very different.
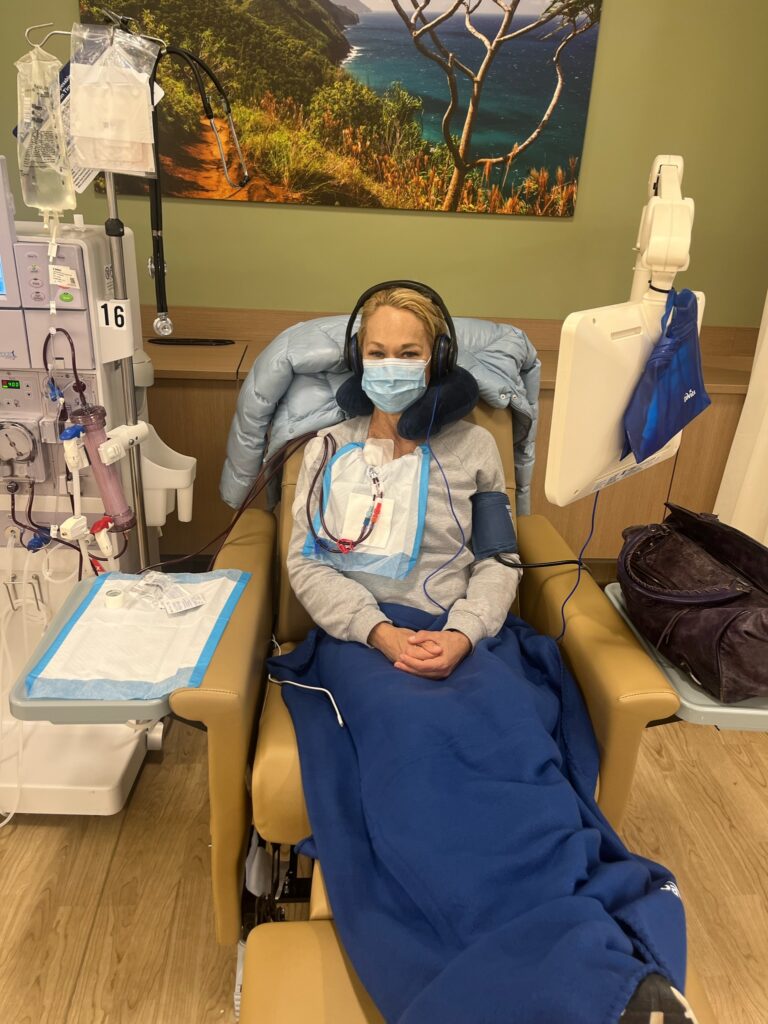
I was now taken to a brightly lit, huge hangar-like room, with multiple chairs seated close by each other. I heard beeping sounds constantly and had very sick patients on either side of me. The personnel were friendly and one nurse offered me a fleece blanket, headphones and a few documents to read in my own time, and then she hooked me up to the machine.
The beeping drove me crazy, so I placed the brittle, plastic headphones over my ears (they barely covered the ear). The chair was one of those recliners that if you move the least, the whole thing goes horizontal; there is no middle step. And the blanket was flimsy, but appreciated. It definitely made me less cold since the environment gave me chills. During my first session, an elderly woman kept crying out “help me” every five minutes, until an ambulance came to pick her up. Next to me was an older man who had issues breathing. I tried to shut my eyes.
When I was done, three hours later, the nurse asked me to weigh myself again (a large scale sits at the entrance) to make sure enough fluid had been “taken off”. I felt wobbly and had a headache that was explained by the “electrolyte shift” that had taken place.
I bravely walked out to be driven home by my mother. I thought about those without family who had to go home by themselves after these sessions. The physical and mental trauma that had taken place do not set one up well up for cooking dinner, or driving a car.
That evening, I was truly exhausted. But the next day, I felt remarkably better! I enjoyed a healthy meal for the first time in quite a while without nausea, could go for a walk without fatigue and generally felt “cleaner”.
Dialysis is, for sure, not worse than death, which is what I had compared it to previously. But I reflect, surely there must be a way to improve the way the treatment is being given to the 550k patients on dialysis in the US?
Three times a week, 12 hrs a week: surely we can work on the setting and the use of time? How about some better chairs, lower light, privacy if wanted, and more sense of community if desired?
Kidney warriors are strong and determined, but we need education about diet, exercise and importantly, ways to get on the transplant list. We also need connections with others.
I hope I can contribute something valuable to the kidney community after spending these weeks in April on dialysis. I pledge to keep trying!
Continue reading part 3 of Karin’s journey: Day of Transplant Surgery
